
Oral systemic health care is no longer a theoretical or emerging concept—it is now a clinically recognized interdisciplinary healthcare model that connects dental health with whole-body medical outcomes. Modern evidence shows that oral diseases such as periodontal infections, gingivitis, and dental caries are strongly associated with systemic health conditions including diabetes mellitus, cardiovascular disease (CVD), respiratory disorders, rheumatoid arthritis, and even adverse pregnancy outcomes.
The mouth acts as both a mirror and a gateway to the body’s internal physiological status. Chronic oral inflammation contributes to systemic inflammatory burden through microbial dissemination and immune-mediated pathways, affecting metabolic and vascular functions beyond the oral cavity.
This comprehensive guide explores the clinical science behind oral systemic health care, the biological pathways involved, disease associations, cost implications, preventive strategies, and why integrated dental-medical collaboration is rapidly becoming essential in modern healthcare systems.
Oral systemic health care refers to the integrated management of oral health conditions as part of overall systemic disease prevention and treatment strategies.
Unlike traditional dentistry—which focuses exclusively on teeth and gums—this model:
Research confirms that oral diseases affect approximately 3.5 billion people globally, disproportionately impacting low- and middle-income populations with limited healthcare access.
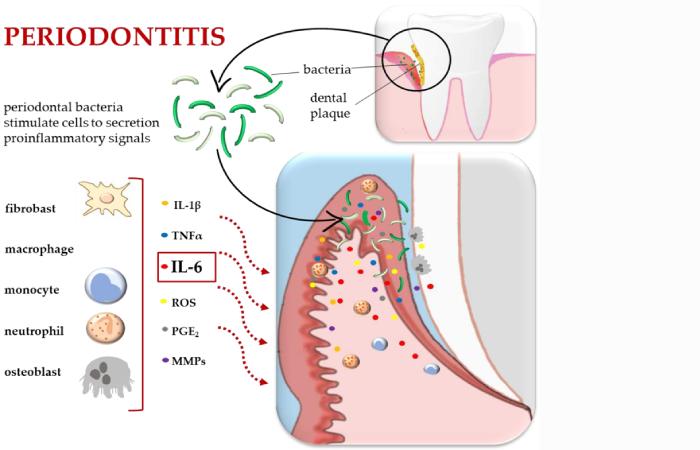
The oral-systemic connection is primarily driven by three pathophysiological mechanisms:
Oral pathogens such as Porphyromonas gingivalis enter the bloodstream through inflamed periodontal tissues, triggering vascular and immunological responses.
Inflammatory mediators such as:
are released during periodontal disease progression and circulate systemically—contributing to endothelial dysfunction and atherogenesis.
Poor oral health worsens glycemic control in diabetic patients, while systemic diseases may impair wound healing and increase susceptibility to periodontal infections—creating a bidirectional disease cycle.
| Oral Condition | Linked Systemic Disease | Mechanism Involved |
| Periodontitis | Cardiovascular Disease | Endothelial inflammation |
| Gingivitis | Diabetes Mellitus | Insulin resistance |
| Dental Caries | Hypertension | Vascular inflammation |
| Oral Infections | Respiratory Disease | Bacterial aspiration |
| Gum Disease | Rheumatoid Arthritis | Immune cross-reactivity |
| Oral Microbiome Imbalance | Adverse Pregnancy Outcomes | Cytokine activation |
Observational studies demonstrate that individuals with chronic diseases such as diabetes or arthritis are twice as likely to require urgent dental treatment compared to those without such conditions.
Chronic periodontal inflammation has been consistently associated with:
Inflammatory mediators and microbial products from periodontal lesions promote platelet aggregation and endothelial activation—key contributors to vascular disease progression.
Clinical studies reveal a moderate statistical association between periodontal disease and glycemic dysregulation, indicating that oral inflammation may directly influence metabolic control.
Periodontal therapy has shown measurable improvements in glycemic control among diabetic patients undergoing dental treatment.
Poor oral hygiene increases the risk of:
Bacteria from the oral cavity can be aspirated into the lungs—particularly in elderly or immunocompromised individuals.
| Healthcare Category | Preventive Dental Care (Annual) | Systemic Disease Treatment (Annual) |
| Routine Dental Cleaning | ₹2,000 – ₹5,000 | — |
| Periodontal Therapy | ₹10,000 – ₹25,000 | — |
| Diabetes Management | — | ₹30,000 – ₹1,00,000 |
| Cardiac Treatment | — | ₹1,50,000 – ₹5,00,000 |
| Hospitalization | — | ₹50,000 – ₹2,00,000 |
Integrated oral systemic care can significantly reduce long-term treatment costs by preventing inflammatory-mediated disease progression.
Key components include:
Routine oral health assessments integrated into chronic disease protocols can improve long-term outcomes for elderly populations and high-risk groups.
| Preventive Practice | Recommended Frequency |
| Dental Check-ups | Every 6 Months |
| Periodontal Screening | Annually |
| Oral Cancer Screening | Annually |
| Salivary Diagnostics | As Required |
Advancements in:
are enabling early identification of systemic diseases through oral health screenings—transforming dentistry into a frontline preventive healthcare discipline.
Interdisciplinary collaboration between dental and medical professionals is now considered essential for translating research evidence into real-world preventive healthcare practices.
Oral systemic health care represents a paradigm shift in modern medicine—recognizing the mouth as an integral component of overall physiological health. The bidirectional relationship between oral diseases and systemic conditions underscores the need for collaborative, preventive, and diagnostic integration between dentistry and general healthcare.
Addressing oral inflammation at an early stage can reduce systemic disease risk, improve metabolic outcomes, lower healthcare expenditures, and ultimately enhance patient quality of life.
As healthcare systems move toward holistic patient-centered care models, oral systemic health care will remain a critical pillar in chronic disease prevention and management.
Syed Sadiq is a health education content researcher who writes evidence-informed guides on symptoms awareness, preventive health habits, and digital safety topics affecting students and families. His articles focus on helping readers understand health-related information clearly before making decisions. Through DionHealthWeb, he publishes structured health-awareness content designed to support informed conversations between readers and healthcare professionals.